Exclusively pumping for twins, triplets or more? Here’s what to do when you are relying on a pump to establish a supply for two or more babies.

This is a guest post by Lindsay Castiglione, an International Board Certified Lactation Consultant with over ten years of experience in supporting families to meeting their feeding goals. She is also the mother of two sets of twins.
I see this scenario over and over in my private practice.
A client is expecting twins or triplets, things were going well with the pregnancy, then suddenly preterm labor begins or a concern at an appointment sends them to the hospital. Sometimes it’s a false alarm and they are sent home, but for others it means an early delivery.
Before they know it, their babies are born and whisked to the NICU – leaving the parents turned upside down emotionally and physically. The thought of establishing a milk supply seems so overwhelming, and sometimes with so much going on, we don’t get off on the right foot.
Or, they were following exclusive pumping guidelines that were really meant for a singleton supply. The parents might be handed a breast pump without much support or helpful instructions and told to pump for their preemies. If they are lucky, get one or two 15-minute visits from a lactation consultant during their hospital stay.
2 or 3 weeks later, they come to me, saying they are struggling to pump enough milk for one baby – let alone two.
Situations like this break my heart, because I often see SO many lost opportunities in the beginning to bring about a more positive outcome. Taking a prenatal Breastfeeding Twins class is so important, as we go over these common challenges and strategies to establish a great supply through them.
Trust me, laying the right supply groundwork from the beginning is much, much preferable to ending up in a situation wishing you had done things differently.
This article will help explain, step-by-step, how to best bring in a supply for twins (or more!) through exclusive pumping. As a mother of 30-weekers who has actually been through this, and also as a board certified lactation consultant, my goal is to help support parents in meeting their feeding goals even when the journey may not look like the way they hoped or anticipated.
You CAN do this, with the right information, strategies, and support.
When reality collides with our hopes and expectations
Circumstances around an early delivery are often emotionally draining and stressful, to say the least. Pumping alone in a hospital room while separated from your babies is likely not at all what you envisioned or hoped for.
Even though it is so hard to make pumping a priority in the aftermath of an early delivery, not stimulating your body to make milk now can have long term effects and substantially limit your future supply.
After our first set of twins were born 10 weeks premature, it was really helpful to frame my mindset in this way:
Making milk for my babies is the best way I can care for them right now. Only I can give them this special milk made exactly for them.
It can be really heart wrenching to recognize that the best physical care your babies can get right now is in the hands of NICU nurses and doctors.
Instead of focusing on that, recognize that pumping as an essential part of their overall care, a superpower only you have. Did you know the milk-making system in our bodies recognize a premature delivery? Our body responds by making milk with extra nutrients and protective factors based on how early they were delivered. Increased immunity boosters help to protect those fragile immune systems, along with extra fat, protein, amino acids, and sodium – all of which fulfill the specific needs of a premature baby.
Providing milk to your babies is more than just nourishment – preterm milk is considered medicinal. Every drop will be custom made, providing exactly what your babies need.
Step One – Using hand expression and pumping to stimulate supply
FAQ – Where do I start?
I just delivered premature twins. My plan was to breastfeed, but now they are in the NICU – where do I start?
As soon as the placenta detaches from the uterine wall, your body flips a hormonal switch into milk-making mode. Because of this, with the appropriate level of stimulation, we can bring in our milk supply whether it is week 25 or week 40.
For the first few days after delivery, expect to see just drops of colostrum when you express – this is normal! Our milk “comes in” or substantially increases in volume generally anywhere from day 2-5.
From as early as an hour or two after delivery, request that a pump (and a staff member who can show you how to use it!) be brought to you.
Getting that first session started ASAP broadcasts the loud and clear message we want to send to your body – “Make that milk!”. The more stimulation we give through pumping (or nursing), the more groundwork our body lays for an abundant future supply.
Aim for 10 sessions of combination hand expression & pumping each day until your milk substantially increases in volume or starts to “come in”.
FAQ – Why both hand expressing and pumping?
“Wait, what? Hand expressing AND pumping? Can’t I do just one?”
For the first few days after delivering, your body is producing small amounts of colostrum, instead of the ounces of milk we might expect when we imagine pumping for our babies.
This is a natural part of establishing any supply, since right after birth a baby is only meant to have tiny feedings of about 1 teaspoon of colostrum at a time. During this short phase, pumping and hand expressing are each going to have their own unique role in this process, and by doing both we will get our supply off to a running start.
Each session should include:
- Hand expression (3-5min on each side) – Best way to collect colostrum or that “liquid gold”, it will be brought to the NICU and provides tons of benefits for the babies.
- Pumping (15-20 minutes) – Fulfills the role of mimicking the babies, providing longer chunks of time to stimulate supply.
Hand expressing colostrum
Colostrum is thicker and more concentrated than transitional or mature milk, and it is easier collected using hand expression.
Think of trying to drink a smoothie from a skinny straw – this is similar to how the suction works with colostrum – it’s just not very effective. Plus, you don’t want to waste any of those drops inside the pump parts where you can’t reach them. Start with spending 5+ min hand expressing each breast followed by 15-20 minutes of pumping with a hospital grade pump.
Hand Expressing Milk by Dr. Jane Morton is a great video on hand expression for a quick lesson on technique. I know it can feel awkward at first!
As you hand express colostrum, carefully collect it in a clean medicine cup, plastic spoon or other appropriate container to be sent to the NICU for your babies.
Every single drop of this colostrum should be used, so make sure you save it and give it to a nurse. If it is only a few drops (not uncommon at all) they can soak it up with a cotton swab and wipe it in their mouths.
Just by doing that, your milk is starting to build their immune system and research shows higher rates of future breastfeeding.
Pumping
After that, we pump. The point of pumping is not in what we collect in the bottles, it is to stimulate the production and increase of your milk supply. With each session, you will activate the hormones prolactin and oxytocin (in charge of building milk supply) and will send the message “We NEED that milk ASAP!” to your body.
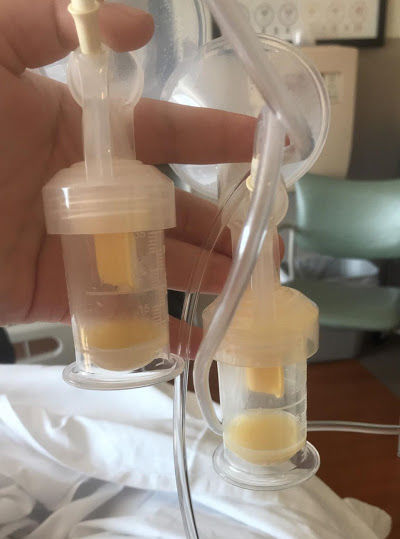
The more pumping/hand expression sessions you fit into the first few days after delivery, the faster your milk will “come in” or substantially increase in volume.
In addition to that benefit, during the first 10 days following the babies’ birth, every time you pump, hand express, or nurse, you are laying the groundwork for your future milk supply. The more you stimulate your prolactin levels, the greater your future capacity of milk production – and not just for now, but research shows us often for the length of your lactation journey.
Different scenarios after birth and moving forward
In my Breastfeeding Twins classes, I often give several versions of the scenarios following delivery. Being able to have your expressing session within hours after delivery and then being able to consistently continue every 2-3 hours around the clock – that would happen under ideal circumstances, or what I call the “sunshine and roses” situation.
Don’t get me wrong, an early delivery and babies in the NICU does not make for a fairytale of any sort, but you get my drift. The reality is, sometimes circumstances beyond our control can temporarily put milk making on the backburner.
The birth of multiple babies can unfortunately come with higher rates of complications during or after the delivery, leading to a disruption in early breastfeeding. Some parents are dealing with their babies being transported to a different hospital, if they needed a more well-equipped NICU. My heart goes out to anyone experiencing situations like this.
If this happened to you, the most important advice I could give, is this:
Don’t stress about what has already occurred when it comes to your milk production. Instead, pretend you are starting over from right now – the sooner you get back on track, the better your results will be. Make a plan to pump 10-12 times over the next 24 hours and focus on moving forward. Stress will not be helpful to your production, and we can’t change what has already happened.
For some of my clients, a disruption in establishing supply presents challenges we eventually must work through with lactation visits. Fortunately, a good IBCLC has lots of proven strategies to help in this situation. It is not that your supply is be doomed, but the earlier we can intercept a lack of stimulation in the first few days, the easier it will be to rebound in the long run.
FAQ – Do I need to pump at night?
“My babies are in the NICU and I am healing from a caesarean delivery. Won’t skipping overnight pumping sessions be more beneficial, so I can heal faster?”
This question comes up a lot, and believe me, I wish I could say to just go ahead and get that sleep! The truth is that overnight sessions are critical to building your supply. Some even say they are the most important sessions of the day.
The overnight hours are when prolactin (the milk-making hormone) is naturally highest. Pumping or nursing will spike your levels which send tons of “make that milk” messages to your body.
I can remember a well-meaning postpartum nurse telling me to skip my overnight session so I could get some sleep, saying helping my body recover would in turn help my milk supply. Unfortunately, that is not the case, and it does make a difference. I had read that this might happen and (albeit, begrudgingly) got up to pump anyway. I definitely saw my hard work pay off and built a great supply, and you can too.
FAQ – Can I use a wearable breast pump?
“I have wearable pump at home, is it fine to use it to exclusively pump with once I am discharged?”
While I 100% understand the allure and convenience of the wearable pumps, to establish a supply with any baby in the NICU, especially twins or other multiples) you would ideally be using a TRUE hospital grade pump.

The pump your insurance supplied you with to keep is (with very rare exceptions) not truly hospital grade. Ask the lactation staff at the hospital about renting one for at least the first 6-8 weeks. Even better would be using the hospital grade pump until your supply is feeding both of your babies without supplementing, after they would be 40w gestationally.
Check with your insurance company as well, ours covered a 90 day rental if the babies were born prior to 36 weeks. Every policy has different coverage though, so calling and asking is your best bet.
If you are ordering a pump from insurance for after supply is well established, the Spectra S1 or S2 and Motif Luna are usually covered fully and great choices. Wearable pumps are clutch in certain circumstances, but generally not for bringing in a supply for multiples or for use as a primary pump if continuing to exclusively pump.
That being said, each pump works differently for each person, so work with an IBCLC if you really need a wearable option that is a good fit for you.
Step 2 – Transitional milk and adjusting your pumping routine accordingly
Two important things usually happen a few days after delivering your preemies – you are discharged from the hospital, and your “transitional milk” makes a grand appearance.
For the babies who have a NICU stay in front of them, discharge day is often really difficult and emotional for the parents. I still remember, in vivid detail, walking down the long corridor of our hospital toward the exit feeling every maternal instinct go haywire as I walked away from my tiny babies. We lived about 45 minutes away from the NICU and it was heartbreaking to be so far from them, even if it was just to sleep, shower, and go back the next day.
At some hospitals, you have the option to stay very close by in a Ronald McDonald house or even at the NICU (if you are super lucky). It is important to plan out your sessions during this transition so that it won’t affect your pumping schedule – it is easy to imagine how this can happen when you have more distractions around.
When your milk comes in, you will suddenly be pumping more and more of this yellowish/white transitional milk. At this point, we are going to make some important shifts to our pumping routine to continue bringing in that optimal twin (or higher order multiples) supply.
Hands-on pumping
While any form of stimulation is great in my eyes, hand expression is now going to be less about manual collection and more about complimenting your pumping routine.
Pumps are powerful machines but they aren’t perfect – often there will be little pockets of milk that are missed. By using your hand to compress and massage before, during, and after your pumping session, you will help to thoroughly empty those missed areas.
Maximizing Milk Production with Hands-On Pumping is a great video from Stanford Medicine with instructions on implementing this skill. Use a hands-free pumping bra that fits securely to hold the flanges, leaving your hands available to compress and massage.
Your pumping schedule
The other adjustment to make (one I don’t hear talked about enough) is to the amount of time you are devoting to a session. Too often, I see clients who were told to pump “15-20 minutes, 8x/day” or a similar recommendation. They follow this diligently but then aren’t producing enough milk for their babies once the feeding volumes have increased.
In my experience, following a pumping schedule dictating a specific number of minutes per session is not the best practice when exclusively pumping for two or more babies.
The focus when bringing in a supply for multiples is to thoroughly and frequently empty your breasts/chest. I have had many clients pump for 15-20min and still have a considerable amount of milk left behind.
Milk production is reliant on the demand being placed on supply – if thoroughly emptied, the body gets the “We’d like more, please!” message. If left full or partially full, “We don’t need all that milk – reduce the supply!” is sent. Unless you are overproducing and need to reign things in a bit, we really do NOT want to send that message.
As far as hard numbers go, the duration & frequency will vary person to person since we don’t all make milk or respond to the pump the same way. I have had a few clients bring in a supply for twins with 8x/day, 15min/session, but for most that just won’t be enough stimulation to signal a supply for more than one baby.
After milk has come in or considerably increased in volume
For a first-time parent of multiples, my typical pumping recommendations are:
Pump 10-12x/day, continuing 3-5 minutes after the last drops of milk, until your output has reached between 55-60oz/day (or more to match your babies’ intake, if that is a greater volume).
You may have tiny babies still in the NICU who are only taking in a fraction of that volume per day, eventually they will be taking the 1-1.5oz/hour full term infants typically need. In the meantime, sit back and watch your stash take over your freezer. As they grow you may need more than 55-60oz/day, but this is a good guideline to start with.
The number of days or weeks it takes to get production up to this point varies widely. If you are an overproducer, you may be pumping 55-60oz by 2 weeks postpartum. For others it may take 6-8 weeks or more.
For some individuals, even with adding the extra 3-5 minutes a plateau can occur, leveling your daily output below what your babies are taking in. So many factors go into this, some of which are frustratingly beyond our control. It’s always best to see an IBCLC if you are struggling to produce, knowing the root cause is the only reliable way to find a remedy.
Step 3: Settling into a consistent routine and maintenance
Once you reach your desired output, slowly reduce the extra minutes over the course of a few days, until you end the session when the last drops are seen. The overall goal is to find the ideal session length(s) for your body that will maintain your desired supply.
You will likely find the time it takes to pump until the last drops will vary from morning to night. This is totally normal, as our milk volume changes throughout the day with hormone fluctuations. A morning session might consistently take 35 minutes for you to empty, but your evening sessions could take 25. It truly is different for every person!
By keeping track of how much milk you are collecting, you will have a useful tool in identifying a consistent and effective pumping schedule. For each session, record the time of day and the amount collected from each side. At the end of the day, add it all up to give you your daily output.
If you notice a consistent dip in your daily output for 2 or 3 days, go back to adding the extra minutes.
Exclusive pumping for multiples sample schedules
10 sessions per day schedule:
- 7am
- 9am
- 11am
- 1pm
- 3pm
- 5pm
- 7pm
- 9pm
- 12am
- 3:30am
12 sessions per day schedule:
- 6am
- 8am
- 10am
- 12pm
- 2pm
- 4pm
- 5pm
- 6pm
- 8pm
- 10pm
- 1am
- 4am
Notice we are spacing sessions differently overnight vs. daytime hours. By pumping more frequently during the day, you can give yourself slightly longer stretches of sleep overnight. If your babies are home from the NICU and you are still exclusively pumping, plan to pump each time they wake for a feeding.
A few other tips
Have your flange sizes checked by the hospital IBCLC, and/or check yourself!
The one or two flange sizes you received with your pump are sort of like guestimates for the general public – in actuality you might need a different size.
The size of your flange is dictated by your nipple size, not your overall breast or areola size. The range of flange sizes available is vast – the largest being 36mm all the way down to a 13mm!
The point of all of this – if you are handed the 24’s in the hospital and they feel either too tight (restricting milk flow) or too large (causing nipple damage & loss of suction), it’s likely you need another size.
Start with the hospital IBCLC and ask for them to check your sizing – which still a good idea if you don’t notice any problems! They may have other sizes at the hospital that they will give you (and bill insurance for), or you may have to purchase them elsewhere.
Having the right size flange is essential when you are exclusively pumping, and especially when you are using the pump to “bring in” a supply for multiples. Incorrect flange size = less emptying = reduced supply. This problem is compounded if we are pumping with the wrong size for the first few weeks, since that is when the supply groundwork is being laid.
The nipple also may change sizes over the course of your pumping experience as well, as your supply and nipples change through your feeding journey.
More info on finding your best flange/breast shield fit here.
Pump at their bedside in the NICU.
Many parents find that volume of milk that they collect in a session is increased when they pump in the NICU. Typically, NICU’s will have hospital grade pumps available for your use, so there is no need to cart your own pump back and forth.
Engaging your senses as much as possible while you pump also helps with volume, so it makes sense that sitting right next to your babies has this same effect. You can smell them, see them, hear them, etc.
I hope you found this article helpful in understanding how to best establish a milk supply for twins, triplets or more using a breast pump.
Lindsay Castiglione is an International Board Certified Lactation Consultant with over ten years of experience in supporting families to meeting their feeding goals. She is also the mother of two sets of twins, a 10-year-old identical boy set born prematurely at 30 weeks, and an 8-year-old boy/girl set born “full term” at 38 weeks. She teaches online prenatal multiples classes, including Expecting Twins, Breastfeeding Twins, and also Breastfeeding Twins for Experienced Parents. Her private practice, Full Hearts Collaborative, provides virtual lactation consultations for twin and triplet parents all over the world. For more information on services and support, please contact her here.
References- Ruth Snyder, Aimee Herdt, Nancy Mejias-Cepeda, John Ladino, Kathryn Crowley, Philip Levy,
Early provision of oropharyngeal colostrum leads to sustained breast milk feedings in preterm infants,
Pediatrics & Neonatology, Volume 58, Issue 6, 2017, Pages 534-540, ISSN 1875-9572 - Morton J, Hall JY, Wong RJ, Thairu L, Benitz WE, Rhine WD. Combining hand techniques with electric pumping increases milk production in mothers of preterm infants. J Perinatol. 2009 Nov;29(11):757-64. doi: 10.1038/jp.2009.87. Epub 2009 Jul 2. PMID: 19571815.
- Bonyata, Kelly. “How does milk production work?” Kellymom. https://kellymom.com/hot-topics/milkproduction/













Leave A Reply!